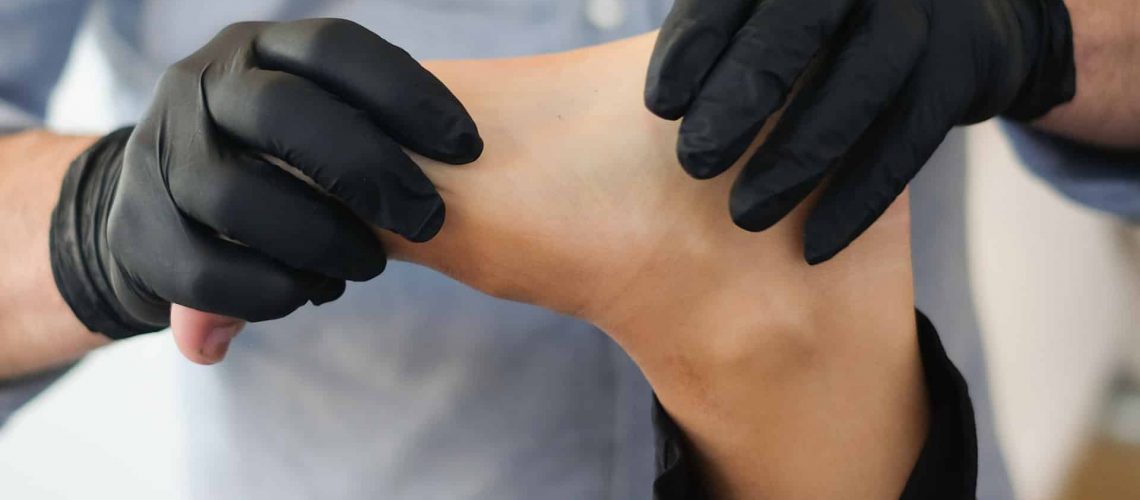
Plantar Fasciitis is one of the top causes of heel pain. It occurs when the thick band of tissue (plantar fascia) that runs across the bottom of your foot–which connects your toes to the heel bone–gets inflamed.
The condition causes stabbing pain, which typically occurs when you first get up in the morning. As you move around, the pain typically decreases. It can return after long periods of standing or when you stand up after sitting.
With the right course of treatment, your pain can be completely eliminated within several months. You can work with your orthopedist to determine the appropriate course of treatment to yield the best results.
Contents
What You Need to Know About Plantar Fasciitis
Symptoms
- Pain while walking or running
- Gradually-developing heel pain
- Sensitivity and sharp pain in the heel — especially in the morning
- Stiffness in the foot
- Sensitivity after sitting for long periods of time, followed by standing
- A bony prominence or heel spur where the plantar fascia attaches to the heel bone
- Warmth, swelling, and tenderness on the bottom of the foot
Causes
The plantar fascia’s shape is that of a bowstring. It supports the arch of your foot, absorbing shock when you walk. When it has too much tension and stress, you can experience small tears in the plantar fascia.
Repeatedly stretching and tearing causes inflammation and irritation. However, the cause of the stretching and tear is often unknown. Underlying diseases can also contribute to the development of the condition.
Diagnosis
Plantar Fasciitis’ diagnosis basis is on the history of the patient’s condition and a physical examination. X-Ray testing can reveal a heel spur, which is commonly related to the condition. It can also eliminate the possibility of other conditions and causes of pain, such as fractures, pinched nerves, or tumors.
Treatment
Plantar Fasciitis treatment consists of a few different options.
- Your doctor might prescribe NSAIDs (nonsteroidal anti-inflammatory medications).
- You can utilize the RICE method (Rest, Ice, Compression, Elevation).
- You can use physical therapy to learn to stretch and strengthen the lower leg muscles, Achilles tendon, and plantar fascia. You can also work with your physical therapist to utilize ultrasonography, massage, and contrast baths to help with longer-term healing.
- Doctors may also give prescriptions for splints or orthotics.
- A steroid injection directly into the most painful part of your plantar fascia. This can ease your pain for roughly a month and will keep the swelling down for longer.
- Changing your shoes could also be beneficial. The recommendation is to wear sports shoes that are soft and comfortable. Custom orthotic shoe inserts can reduce irritation of the inflamed tissues. They can reduce the excess motion of the foot and decrease strain to the plantar fascia.
If the pain doesn’t diminish after treatment, your orthopedist may order a plantar fascia release — a surgical procedure that involves cutting part of the plantar fascia ligament to release tension and relieve inflammation. Surgery is rare but is sometimes necessary.
Your orthopedist may also recommend shock-wave therapy that shocks your plantar fascia using sound waves to help stimulate blood flow and heal the tissue. The shock waves also stun your nerves and help to reduce your pain.
Prognosis
Plantar Fasciitis usually resolves itself with conservative methods, like RICE and taking over-the-counter medications. Rarely the condition evolves into a more serious condition, known as plantar fasciosis. Plantar fasciosis responds to very different treatments than plantar fasciitis.
Risk Factors
Plantar Fasciitis often develops without a known cause, but several risk factors make it more likely for you to develop the condition.
- Being between the ages of 40 and 60.
- Exercises that put high stress on your heels.
- Being overweight or obese.
- Flat feet, high arches, or odd walking patterns.
- Spending an excessive amount of time on your feet.
Complications
Ignoring the condition can cause chronic heel pain that affects your routine. Altering the way you walk when you have the condition can lead to further problems with your feet, back, heels, and more.
Chronic plantar fasciitis (over one year) becomes chronic due to the plantar fascia’s avascular scarring. It is increasingly painful because of the low blood supply to the scarred tissues and resists treatment that reduces inflammation. Talk to your doctor if you are experiencing chronic heel or foot pain.
Prevention
You can help prevent plantar fasciitis by treating any underlying associated inflammatory disease and wearing proper footwear and shoe inserts. Stretching can also help.
Let Us Help
If you’re looking for the best orthopedic care in the Gillette or Douglas areas, look no further than Thunder Basin Orthopedics and Sports Medicine.
Treating everything from fractures and traumatic injuries to joint replacement, plantar fasciitis, and sports injuries, Thunder Basin Orthopaedics and Sports Medicine gives individualized treatment using a variety of techniques to operate with less damage to the body.
Looking for the skilled staff and top surgeons to get you back on your feet and back in the game? Contact Thunder Basin Orthopaedics and Sports Medicine today. You can also find new patient paperwork here to get a head start on your orthopedic needs!